|

Dermatologic Applications of
the Erbium: YAG Laser
Author:
Philip S.H. Hughes, M.D.
Diplomate, American Board of Dermatology
San Antonio, Texas
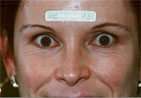
| Figure
1. |
Periorbital rhytids, before (A) and
6 days after (B) Erbium:YAG laser resurfacing. Note rapid resolution
of erythema. (photos submitted by Philip Hughes, M.D.) |
 |
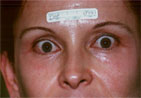 |
| Figure 2. |
Periorbital rhytids in type IV skin,
before (A) and 7 weeks after (B) Erbium:YAG laser resurfacing.
Note absence of postinflammatory hyperpigmentation.(photos submitted
by Philip Hughes, M.D.) |
 |
 |
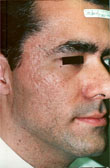
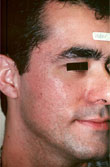
| Figure 3. |
Acne scars in type IV skin, before
(A) and 10 weeks after (B) Erbium:YAG laser resurfacing. Note
absence of postinfiammatory hyperpigmentation. (Photos submitted
by Philip Hughes, MD) |
 |
 |
Overview
The Erbium:YAG laser (Continuum Biomedical, Dublin,
CA), emitting in the infrared at the 2.94 micron peak of the water
absorption spectrum, produces minimal residual thermal damage (2
microns at 4.2 joules/sq.cm.) compared to superpulsed C02 lasers
(greater than 100 microns). This means there is less pain (procedures
can be done with no anesthesia or topical EMLA), faster healing,
and faster resolution of erythema with the Erbium:YAG laser compared
to the carbon dioxide laser. Specifically, facial resurfacing procedures
with the Erbium:YAG laser re-epithelialize in 5 days and erythema
generally resolves in 5 days! Using a fluence of around 5 joules/sq.cm.
the Erbium:YAG laser penetrates 25-30 microns per pulse. The first
pulse is intraepidermal. After the second pulse the epidermis is
ablated and the upper papillary dermis is entered.
Indications
Extrinsic photoaging produces rhytids, actinic keratoses,
and solar elastosis, all of which are effectively treated with the
Erbium:YAG laser.
Intrinsic aging (producing the sagging skin of blepharochalasia
or the jowling of dermatochalasia), infraorbital fat pads or deep
wrinkling from muscular contraction are not appropriate candidates
for Erbium:YAG resurfacing.
Do not use ablative methods (including Erbium:YAG
resurfacing) for melasma or postinflammatory hyperpigmentation.
These procedures frequently exacerbate the problem.
Epidermal tumors (such as actinic keratosis, seborrheic
keratosis, lentigo, verruca vulgaris, molluscum contagiosum, achrocordon,
leukoplakia), selective elevated dermal tumors (like syringoma ,sebaceous
hyperplasia, xanthelasma, cherry angioma, dermal nevus, steatocystoma
multiplex), rhinophyma and superficial basal cell epithelioma may
all be ablated with the Erbium:YAG laser. (Be sure to consider the
need for histopathology before using an ablative procedure on a
tumor.)
Scars, such as acne scars (deep pitted scars should
be punch-stitched and resurfaced 6 weeks later), varicella scars,
traumatic scars and surgical scars (ideal resurfacing time is 4-6
weeks post-op) are all improved with the Erbium:YAG laser. Hypertrophic
scars or keloids (especially if followed by 585 nm pulse dye laser
treatment or intralesional corticosteroid injections) are candidates
for Erbium:YAG ablation. Mature “spread” scars may be
de-epithelialized with the Erbium:YAG laser and then treated with
the 585 NM pulsed dye laser.
Furthermore, an experimental use of the Erbium:YAG
is upper epidermal ablation to enhance the penetration of topical
drugs.
Contradictions
Although controversial, from a medical legal standpoint
alone, wait 6 months after Accutane before a resurfacing procedure.
Avoid patients with keloids or vitiligo. With ectropion, don't do
eyelid work. Because of the presumed hazard of the laser plume,
don't use the laser in the presence of HIV.
Flammability hazards of the Erbium:YAG laser
At 5-10 herz with a 5 mm spot size, a dry cotton ball
will burst into flame. At atmospheric oxygen, the following have
not flamed: cotton balls soaked in 70% isopropanol, cotton drapes,
paper drapes, human hair.
Equipment
- Room exhaust
- Smoke evacuator (e.g., Acu-Evac 1-800-327-0015)
- Fire extinguisher
- Wet towel
- Patient eye protection: wet gauze, Cox eyeshields
(internal or external), Jaeger plate (Oculo-Plastik, Montreal,
1-888-381-3292)
- Opthaine drops
- Refresh PM & Refresh liquid
- Patient tooth protection: wet gauze, athletic mouth
guards, stainless steel mouth guards (a tooth, even with a film
of saliva on it, will be etched by the Erbium:YAG laser)
- Operator eye protection
- Surgical masks
- 35% aqueous aluminum chloride solution (try to
avoid, delays healing)
- Aquaphor Healing Ointment
- Spenco 2nd Skin
- Flexinet (Genetic Labs 1-800-328-2634)
Patient Anesthesia
Use pre-op sedatives or minor tranquilizers and oral
analgesia. I use Valium 10-15 mgm and two Tylenol #3 with codeine
(may substitute 2 Vicodin tablets) 1 hour before resurfacing.
Apply EMLA cream to defatted skin (scrub with soap
and water, wipe with 70% iosopropanol). Apply a thick "white"
layer and occlude with Saran wrap. Lightly tape in place with paper
tape. Keep the patient lying down so that the Saran wrap doesn't
slide down. Consider doing this in your office properly, so it works!
With multiple passes, the procedure is moderately
unpleasant but tolerable. In over 400 consecutive cases, I have
not needed or used infiltration anesthesia, nerve blocks, or IV
sedation.
There are three supplemental topical anesthetic modalities
that may be employed during a resurfacing procedure. One, after
I pass with the Erbium:YAG laser, EMLA may be applied; wait 60 seconds
and effective deeper anesthesia is obtained. Don't try this after
more than 1 pass as it will sting severely. Second, after any number
of passes, squirt a pH-neutralized solution of 10 parts 1% lidocaine
with epinephrine and 1 part 8.4% sodium bicarbonate onto the skin
between passes, wait 60 seconds, and obtain analgesia. Wipe dry
before proceeding with resurfacing, because the aqueous solution
will absorb the laser energy. Third, 5% Xylocaine ointment ("plain,"
nonflavored) is effective and causes minimal discomfort when applied.
No anesthesia is required for removal of isolated
lesions or small scar resurfacing. Biophysics
The Erbium:YAG fires almost silently. The "pop"
with each pulse is from the supersonic ejection of tissue. The higher
the fluence, the louder the "pop." Note the build-up of
"cotton candy" on the handpiece. With higher fluence,
there is a minimal insignificant increase in residual thermal damage.
There is greater ablation per pulse and slightly prolonged healing
time and erythema with higher fluence. The ablation threshold is
about 1.5 joules/sq.cm. for human skin.
Using one of my child's old deciduous tooth, one pulse
with the Erbium:YAG laser permanently etched the tooth, even with
saliva on it.
The 5mm spot size produces a columnated beam. The
2mm and the 3.5mm handpieces produce a focused beam, the diameter
gets larger and the power (joules/sq.cm.) lessens as the distance
is increased beyond the “guide.” With the 2mm spot size,
at 6 inches or so from the skin there is almost no power delivered
to the skin target (the power is below the ablation threshold of
the skin). This is because the beam diverges. (It is not due to
water vapor in the air, as water vapor, in contrast to liquid water,
is essentially transparent to 2.94 micron wavelength light.)
Preoperative Care
In general, start all resurfacing patients on Retin
A and LacHydrin 1 month before the procedure. This speeds up re-epithelialization
and probably lessens the incidence of postinflammatory hyperpigmentation.
In darker skin types, I will sometimes add a topical hydroquinone
product to the regimen, again to lessen the likelihood of postinflammatory
hyperpigmentation. Recommend sunscreens.
All patients are started on an oral anti-herpes simplex
medication the morning of the procedure. My current favorite is
Valtrex.
Technique
Use eye and tooth protection for the patient. The
operator and assistant need laser-safe eyewear and facial masks.
Due to presumed hazards of the laser plume, use a smoke evacuator.
For isolated lesions, use the 2 mm (at 175 mj) or
3.5 mm handpiece (at 450 mj) to ablate epidermal lesions. With macular
epidermal lesions, 2-4 passes will produce visible ablation below
the basement membrane to the pinkish upper papillary dermis. With
experience, this endpoint is readily recognized.
Elevated dermal tumors (syringomas, sebaceous hyperplasia)
are ablated until they are flush with the epidermis.
On a few occasions, I have treated hypertrophic actinic
keratoses, superficial squamous cell carcinoma or superficial basal
cell carcinoma by a technique of repeated Erbium:YAG vaporization
followed by rubbing with a gauze, reminiscent of “electrodessication
and curettage.”
Leukoplakia of the lower lip (after a shave biopsy
result is back) is treated with 4-6 passes with the 5mm handpiece
at 935 mj at 5 herz.
For resurfacing larger areas (rhytids, scars), use
the 5mm handpiece (935 mj) at 5 herz around the eyelids, glabella,
nose and mouth. Speed up to 10 herz for the cheeks and forehead.
No wiping of treated tissue is required; the tissue is literally
ejected in tiny fragments at supersonic speeds, producing the "popping"
sound.
I do 3-4 passes for the lower eyelids, 7-9 passes
for the glabella and peri-oral areas, and5-7 passes everywhere else
on the face. If needed, I will use a 2 mm handpiece (at 175mj) after
the above passes for selective "sculpting" of the shoulders
of acne or varicella scars. I gently pull the wrinkled skin while
resurfacing, thus enhancing the ablation of the shoulders and valleys
of rhytids.
When resurfacing, after 2 passes (when the upper papillary
dermis is entered), I can't determine depth, so I count the number
of passes. Because there is very little residual thermal damage
(10 microns or less) with the Erbium:YAG laser at the fluences used,
there is no color change as deeper dermal areas are entered. Focal
bleeding or wrinkle or scar ablation are other end-points.
By the way, the apparent wrinkle or scar ablation
seen immediately is temporary. The defects reappear after a few
minutes, suggesting that the temporary ablation is really dehydration
of tissue.
Bleeding is not a problem with resurfacing. Sometimes,
when ablating isolated lesions, bleeding will occur. This can be
stopped with pressure or 35% aqueous aluminum chloride solution.
Aluminum chloride solution delays wound healing, so use it only
if needed.
A "combined" technique is used for non-erythematous
mature "spread" or hypertrophic scars (typically pre-auricular
and post-auricular spread scars following a facelift) consisting
of 3 passes with the Erbium:YAG laser (5mm spot size at 935 mj)
followed with 585 NM pulsed dye laser treatment (10 mm spot size
at 3.0 to 3.4 joules/sq.cm.) Focal sculpting passes may be made
with the Erbium:YAG (2mm spot size at 175 mj) to elevated areas
prior to the pulsed dye surgery.
Postoperative care
For individual lesions, occlude with Aquaphor Healing
Ointment and a bandage daily. Clean with shower water. Avoid hydrogen
peroxide, as this delays wound healing.
Immediately after resurfacing of larger areas, cover
the treated area with AquaphorHealing Ointment. Compress the treated
area 3x daily with a solution of 1 tsp. Betadinesolution (not cleanser)
in 1 cup of water. Then cover with Aquaphor Healing Ointment. Shower
water is OK. On the 4th day, clean with Cetaphil Cleansing Lotion
and apply the Aquaphor afterwards until healed. Avoid topical antibiotics
due to the high incidence of allergic contact dermatitis following
resurfacing.
For cheek resurfacing (where there is less movement),
I like Spenco 2nd Skin or Vigilon held in place with Flexinet the
first 24 hours. On the 2nd day, start the above compresses and ointment.
I do not routinely prescribe oral or topical antibiotics
or antifungals.
Edema is generally not a significant problem following
Erbium:YAG resurfacing; however, sometimes after full facial or
eyelid resurfacing, I will use p.o. prednisone 20 mgm. immediately
post-op and another 20 mgm. h.s. to lessen edema.
Restart Retin A and LacHydrin on the 10th day. Use
sunscreens.
Following a period of dermal remodeling, touch-up
resurfacing may be done 6 to 8 weeks later.
Healing Rates
Facial resurfacing consistently re-epithelializes
in 5 days and erythema generally resolves in five days.
Dorsal hand and forearm lesions will epithelialize
in 7-9 days if occluded, 14 days if not occluded. Erythema lasts
about 30 days.
Leukoplakia of the entire lower lip responds to Erbium:YAG
ablation and heals in 3 weeks without scarring.
Postinflammatory hyperpigmentation is rare, particularly
with the use of Retin A and occasionally hydroquinone preoperatively.
Complications
In 400 individual cases. I have had I case of culture-proven
bacterial pyoderma (staph. aureus) which responded to Zithromax
treatment. There have been several cases of persistent erythema
(greater than 4 weeks); one followed a severe wind and sunburn 5
days after resurfacing multiple facial actinic keratoses. Several
patients have developed a superficial folliculitis (acneiform eruption)
primarily in adjacent areas, perhaps due to Aquaphor occlusion.
One patient, suffering from acne excoriee' (neurotic excoriations),
excoriated an Erbium:YAG resurfaced postsurgical scar 2 weeks after
resurfacing (the scar was secondary to excision of a deep scar produced
by self-induced excoriation). An identical scar on the other side
of her chin, healed uneventfully following resurfacing.
Several cases of Polysporin dermatitis occurred. Three
weeks after resurfacing pen-orbital rhytids, one patient developed
transient (3 days) pinpoint purpura of the treated eyelids and lateral
canthal area. There was one erythematous flat scar at the site of
a facial actinic keratosis ablated 2 months earlier.
I have had one case of herpes labialis post-resurfacing,
despite the patient taking Valtrex 500 mgm b.i.d. x 7 days starting
the morning of the procedure
If there is a problem, consider herpes simplex, bacterial
pyoderma, candidiasis and allergic contact dermatitis. If the KOH
exam is negative, pending bacterial and fungal cultures, start Zithromax.
Do open patch tests to Aquaphor and Betadine solution (apply twice
daily for 2 days to dime-size areas on the forearm).
As mentioned, postinflammatory hyperpigmentation is
rare.
Cutaneous Contraction
With Erbium:YAG laser resurfacing there is an immediate
and persistent 4% contraction of the skin followed by a 13% contraction
which then develops over a 2-3 week period. This contraction persisted
during a 11 week period in one study (Philip Hughes, submitted for
publication).
Results
Epidermal lesions ablated with the Erbium:YAG laser
healed without scarring or prolonged erythema, except as mentioned
under "complications."
Ablation of sebaceous hyperplasia produces "practically
perfect" results. And never before has there been a successfiil
method for syringoma ablation.
In general, rhytids and acne scars resulted in 50%
improvement following Erbium:YAG resurfacing. With rhytids, improvement
was usually observed 3 weeks post-op. Importantly, acne scars continue
to improve for many months following resurfacing. Specifically,
in evaluating my series of rhytids resurfaced with the Erbium:YAG
laser, 45% of results were "excellent," 42% “good,”
3% “fair,” and 10% "unknown" (too soon to evaluate).
In rating acne scar improvement following Erbium:YAO resurfacing,
22% were rated "excellent," 33% "good," 33%
"fair," and 11 % "unknown (too soon to evaluate).
Varicella scars were dramatically improved, 75% improvement
occurring with 1 treatment.
Patient satisfaction
Comparing liquid nitrogen cryosurgery to Erbium:YAG
ablation of individual tumors, patients prefer the laser. It is
less painful during the procedure and heals faster.
Patients who have experienced 35% combined TCA peels,
dermabrasion, and Erbium:YAG resurfacing (I have several who have
experienced all three), find the laser resurfacing the least unpleasant,
both during the procedure and postoperatively.
Following ErbiumYAG resurfacing of one area of the
face, it is common for patients to comment during post-op visits
about other facial areas that they want treated. Patients commonly
refer friends and relatives for Erbium:YAG resurfacing.
Myths
One common misconception is that the Erbium:YAG laser
does not ablate deeply. In fact, the laser ablates 25-30 microns
of tissue per pulse. For example, after 7 passes, about 200 microns
are vaporized. There is still minimal residual thermal damage (3
microns) below this 200 micron ablation.
Another controversy or misconception is whether or
not deep thermal damage is required for permanent collagen shrinkage.
This appears unimportant, since with Erbium:YAG resurfacing, I have
mentioned there is immediate and persistent 4 % cutaneous contraction.
Then after 1 -2 weeks a 13% tightening occurs which persists through
a 11 week observation period.
Philip Hughes, M.D.
San Antonio, Texas
(revised 6/10/97)
|